
It’s never a pleasant experience when that throbbing toothache won’t let you sleep or that jabbing pain catches you while you’re eating. You might be trying to tell yourself it will go away or it isn’t serious. However, your body might actually be warning you that it’s time for a root canal. If you are experiencing severe tooth pain, a root canal may be necessary to save your tooth. Getting regular dental checkups is one of the best ways to determine if you need a root canal before the damage becomes severe. Every day, across the U.S. and right here in Murrieta, patients ignore the symptoms of an infected tooth for too long—and come in to see us with much larger problems that could have been prevented. Here are seven signs you need a root canal.
Key Takeaways
- Persistent, throbbing tooth pain lasting days or worsening over time often signals infected or inflamed inner pulp tissue.
- Lingering sensitivity to hot or cold temperatures beyond a few seconds may indicate compromised nerve tissue inside the tooth.
- Swollen gums, pimple-like abscesses, or discoloration can signal spreading infection requiring prompt root canal treatment.
- Pain when chewing or touching a tooth, or a cracked tooth, may expose pulp to bacteria causing infection.
- A root canal removes infected pulp, cleans the tooth, and prevents further infection, potentially saving the natural tooth.
7 Signs You May Need a Root Canal
(1) Persistent Tooth Pain
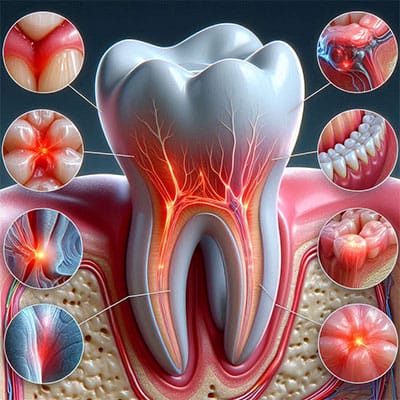 Persistent tooth pain is one of the most common warning signs that you may need a root canal. While occasional tooth discomfort can result from temporary sensitivity or minor irritation, pain that continues for days or worsens over time often indicates a more profound problem inside the tooth. The inner portion of the tooth — known as the pulp — contains nerves and blood vessels. When this tissue becomes infected or inflamed due to deep decay, cracks, trauma, or repeated dental procedures, it can cause constant or severe pain. Many patients describe root canal pain as throbbing, sharp, or pressure-like. The discomfort may intensify while chewing, biting down, or consuming hot and cold foods and beverages. In some cases, the pain may spread to the jaw, ear, or surrounding teeth. Ignoring persistent tooth pain can allow the infection to worsen and potentially spread into the gums or jawbone. A root canal procedure removes the infected pulp, cleans the inside of the tooth, and seals it to prevent further infection. Early treatment can relieve pain, save the natural tooth, and help avoid more extensive dental procedures such as extraction or dental implants.
Persistent tooth pain is one of the most common warning signs that you may need a root canal. While occasional tooth discomfort can result from temporary sensitivity or minor irritation, pain that continues for days or worsens over time often indicates a more profound problem inside the tooth. The inner portion of the tooth — known as the pulp — contains nerves and blood vessels. When this tissue becomes infected or inflamed due to deep decay, cracks, trauma, or repeated dental procedures, it can cause constant or severe pain. Many patients describe root canal pain as throbbing, sharp, or pressure-like. The discomfort may intensify while chewing, biting down, or consuming hot and cold foods and beverages. In some cases, the pain may spread to the jaw, ear, or surrounding teeth. Ignoring persistent tooth pain can allow the infection to worsen and potentially spread into the gums or jawbone. A root canal procedure removes the infected pulp, cleans the inside of the tooth, and seals it to prevent further infection. Early treatment can relieve pain, save the natural tooth, and help avoid more extensive dental procedures such as extraction or dental implants.
(2) Extreme Sensitivity to Hot or Cold
Extreme sensitivity to hot or cold temperatures can be a major warning sign that you may need a root canal. While mild tooth sensitivity is common and may result from worn enamel or minor gum recession, intense or lingering pain after consuming hot coffee, cold drinks, soup, or ice cream may indicate damage deep inside the tooth. This type of sensitivity often occurs when the pulp becomes inflamed or infected. Healthy teeth typically react briefly to temperature changes and then return to normal. However, when discomfort lasts for several seconds or even minutes, it can signal that the inner nerve tissue has been compromised. Deep cavities, cracked teeth, trauma, or repeated dental procedures can expose the pulp to bacteria and trigger inflammation. As the infection progresses, sensitivity may become more severe and eventually develop into constant tooth pain or swelling. A root canal removes the infected pulp, disinfects the inside of the tooth, and seals it to prevent future infection. Learn when to seek professional help for teeth sensitivity.
(3) Swollen or Tender Gums
Swollen or tender gums around a specific tooth can be a strong indication that you may need a root canal. When bacteria enter the inner pulp through deep decay, cracks, or injury, an infection can develop inside the root canals. As the infection spreads, the surrounding gum tissue may become inflamed, swollen, painful, or sensitive to touch. In some cases, patients notice a small bump or pimple-like abscess on the gums near the affected tooth—a sign of a serious dental infection. Swelling may also be accompanied by tooth pain, foul breath, or increased sensitivity to hot and cold foods. Ignoring swollen gums caused by infection can allow bacteria to spread deeper into the jawbone and surrounding tissues.
(4) Darkening or Discoloration of the Tooth
Darkening or discoloration of a tooth can be a sign that the inner pulp has been damaged or infected, which may require a root canal. When the nerve and blood vessels inside a tooth begin to die due to trauma, deep decay, or infection, the tooth may gradually turn gray, brown, or darker than surrounding teeth. Unlike surface stains caused by food or drinks, this type of discoloration originates from inside the tooth itself. Often, discoloration is accompanied by pain, sensitivity, or swelling. A root canal removes the damaged pulp and helps save the natural tooth while preventing the infection from spreading to nearby tissues or bone.
(5) Pain When Chewing or Touching the Tooth
Pain when chewing or touching a tooth can be a sign that the inner pulp is inflamed or infected. When bacteria reach the nerves inside the tooth through deep decay, cracks, or trauma, pressure from biting or chewing can irritate the damaged tissue and cause sharp or throbbing pain. In some cases, the tooth may also feel tender when touched or exposed to temperature changes. A root canal removes the infected pulp, relieves discomfort, and helps save the natural tooth from extraction.
(6) A Cracked or Chipped Tooth
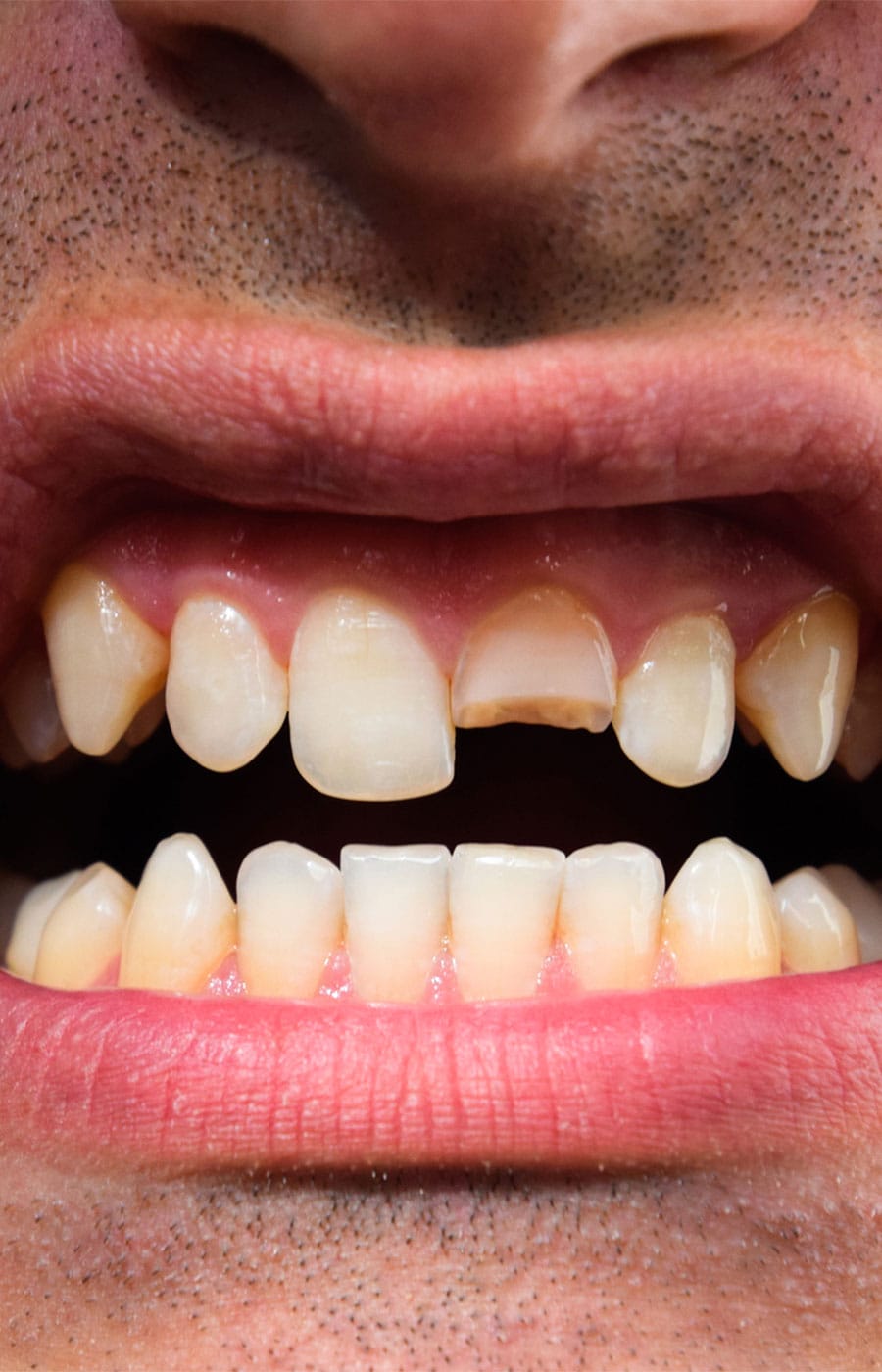 A cracked or chipped tooth can expose the sensitive inner pulp to bacteria, increasing the risk of infection and the need for a root canal. Even small cracks may allow germs to enter deep inside the tooth, causing inflammation, pain, and damage to the nerves and blood vessels. Patients may experience discomfort while chewing, sensitivity to hot or cold temperatures, or swelling around the affected tooth. If left untreated, the infection can spread and weaken the tooth further. A root canal removes the infected pulp, disinfects the inside of the tooth, and helps preserve the natural tooth while preventing more serious dental complications or extraction.
A cracked or chipped tooth can expose the sensitive inner pulp to bacteria, increasing the risk of infection and the need for a root canal. Even small cracks may allow germs to enter deep inside the tooth, causing inflammation, pain, and damage to the nerves and blood vessels. Patients may experience discomfort while chewing, sensitivity to hot or cold temperatures, or swelling around the affected tooth. If left untreated, the infection can spread and weaken the tooth further. A root canal removes the infected pulp, disinfects the inside of the tooth, and helps preserve the natural tooth while preventing more serious dental complications or extraction.
(7) A Persistent Pimple on the Gums
A persistent pimple on the gums — sometimes called a gum boil or dental abscess — is often a sign of an infected tooth that may require a root canal. It forms when bacteria from an infected tooth pulp spread into the surrounding tissue. It may release pus or fluid and can be accompanied by pain, swelling, bad breath, or a bad taste in the mouth. Even if the bump temporarily disappears, the infection usually remains active beneath the surface. A root canal removes the infected pulp, cleans the inside of the tooth, and helps eliminate the infection while preserving the natural tooth.
Identifying and Addressing Infected Tooth Symptoms
Spotting infected tooth symptoms is probably the best thing you can do for your oral health. Pain is the most common sign. If your tooth hurts long after exposure to hot/cold foods or liquids, it could be infected. Sensitivity from an infected tooth can feel deep and throbbing—rather than normal sensitivity. Swelling at the gum line, jaw, or even your face is another big sign that the infection is spreading. Tender lymph nodes in your neck are also a cause for concern. A change in tooth color, increased sensitivity when biting, or a pimple-like sinus tract on your gums near the painful tooth are all warning signs.
💡 Root canal treatment in Murrieta, CA: Our dentists will remove the infected pulp with a thorough cleaning, seal the tooth, and have it safe to use for many years.
Impact of Infected Tooth Symptoms on Overall Health
Symptoms of an infected tooth don’t stay contained to just that tooth. You can end up damaging other teeth, your gums, and your jaw, and even cause issues throughout your whole body when you ignore problems like this. The infection can spread to other areas of your gums and cause gum disease. As the infection destroys bone around your tooth, nearby teeth can shift — leading to crooked teeth or bite issues that may require braces or other dental work to correct. Studies have also linked oral inflammation to heart disease, diabetes, and lung issues. This is why dentists say: your mouth is a reflection of your body’s health.
⚠️ Don’t wait: An untreated dental infection can spread to the bloodstream and reach the heart, lungs, and even the brain. In severe cases, sepsis can be life-threatening.
Lifestyle Habits That Increase Root Canal Risk
 Unhealthy habits cause many root canals, but lifestyle changes can prevent them. Diet & Sugar: Eating lots of sweets and high-acid foods causes decay. As decay progresses into the tooth, it can reach the pulp, requiring a root canal. Oral Hygiene: Brush twice a day, floss daily, and visit your dentist regularly to prevent plaque and bacteria buildup. Teeth Grinding: Grinding or clenching can crack your tooth, allowing bacteria to reach the pulp. Tobacco & Alcohol: Smoking or using chewing tobacco greatly increases the risk of gum disease and infections. Drinking too much alcohol causes dry mouth, leaving you more susceptible to decay-causing bacteria.
Unhealthy habits cause many root canals, but lifestyle changes can prevent them. Diet & Sugar: Eating lots of sweets and high-acid foods causes decay. As decay progresses into the tooth, it can reach the pulp, requiring a root canal. Oral Hygiene: Brush twice a day, floss daily, and visit your dentist regularly to prevent plaque and bacteria buildup. Teeth Grinding: Grinding or clenching can crack your tooth, allowing bacteria to reach the pulp. Tobacco & Alcohol: Smoking or using chewing tobacco greatly increases the risk of gum disease and infections. Drinking too much alcohol causes dry mouth, leaving you more susceptible to decay-causing bacteria.
The Dangers of Ignoring a Dental Abscess
A dental abscess is something every person dreads. Symptoms include throbbing pain that spreads, drainage of pus inside the mouth, a bad taste that won’t go away, and swelling in the face or neck. The infection will not remain contained to your mouth forever. Bacteria can travel through the bloodstream to your heart, lungs, and even brain. An abscess won’t heal on its own — it will continue to eat away at bone and surrounding tissue until your tooth falls out or needs to be extracted.
Treatment: The most common treatment for a dental abscess is root canal therapy. During the procedure, the dentist removes the infected pulp, cleans and disinfects the canals, and seals the tooth. If the infection is severe, antibiotics may be prescribed as well.
The Psychological Impact of Severe Tooth Pain
One thing people often overlook is the psychological impact of chronic tooth pain. Persistent toothaches can cause lost sleep, difficulty concentrating, irritability, and social withdrawal. Chronic pain puts you at greater risk for anxiety and depression. Root canals are done under local anesthesia and are no more uncomfortable than an average filling. After treatment, the cause of your pain is gone. Many patients report that it wasn’t just a relief for their tooth — it was a relief for their mental health as well. All Murrieta root canal dentists understand anxiety and will work with you to make you as comfortable as possible. Sedation is always an option for nervous patients.
Conclusion
Healthy teeth can last a lifetime, but only with proper care and attention. Understanding these seven key signs you may need a root canal will help you better care for your smile: severe tooth pain that won’t go away, temperature sensitivity, swelling, tooth discoloration, the presence of a dental fistula, pain upon biting down, and abscess symptoms. Dismissing your symptoms won’t make them go away. Letting an issue go from treatable to emergency can have life-threatening consequences. Root canal treatment isn’t something to fear — in fact, it’s one of the most effective ways to rid your body of infection, gain relief from severe tooth pain, and save your natural smile. Whether you’re looking for root canal treatment in Murrieta or just wondering what’s causing that nagging toothache, the best thing you can do is call your dentist today. Your oral health is your overall health, and getting treatment early is always the smartest and kindest decision you can make.
FAQs
What is the most common sign you need a root canal?
Persistent, throbbing tooth pain that lasts for days or worsens over time is the most common warning sign of an infected or inflamed tooth pulp requiring a root canal.
Why does tooth sensitivity indicate a root canal is needed?
Lingering sensitivity to hot or cold temperatures beyond a few seconds may signal that the inner nerve tissue has been compromised by infection or inflammation.
What causes swollen gums near a tooth?
Swollen or tender gums around a specific tooth often indicate that bacteria have infected the inner pulp and spread into surrounding gum tissue.
Can a discolored tooth mean you need a root canal?
Yes. A tooth turning gray or brown may indicate the inner pulp has died due to trauma or infection, often requiring a root canal.
Why does chewing cause pain with an infected tooth?
Pressure from chewing irritates inflamed or infected pulp tissue, causing sharp or throbbing pain, especially when bacteria have reached the inner nerves.
Can a cracked tooth lead to a root canal?
Yes. Even small cracks can allow bacteria to enter the pulp, causing infection, inflammation, and nerve damage that may require root canal treatment.
What is a pimple on the gums a sign of?
A persistent gum pimple, or dental abscess, signals an active tooth infection that typically requires a root canal to remove infected pulp and eliminate bacteria.
What does a root canal procedure actually do?
A root canal removes infected pulp, cleans and disinfects the inside of the tooth, and seals it to prevent further infection while preserving the natural tooth.
Can a tooth infection spread to other areas?
Yes. Untreated infections can spread to the jawbone, gums, neck lymph nodes, and surrounding tissues, making early treatment critical.
When should you see a dentist about tooth pain?
You should see a dentist if tooth pain persists for more than a few days, worsens, or is accompanied by swelling, sensitivity, or gum abnormalities.


